Proven at Scale Across States and Providers

26 States Use Our Program

130,000+ Currently Being Monitored


The Health Risk Screening Tool (HRST®) is a validated health risk screening and stratification instrument designed for people with intellectual and developmental disabilities (IDD) and other at-risk populations. It enables organizations to identify, quantify, and proactively manage health risks that can lead to destabilization, adverse outcomes, avoidable suffering, and premature mortality.
The HRST is a proprietary, HIPAA-compliant, web-based instrument that applies a standardized methodology to generate a Health Care Level (HCL)—a clinically reliable measure of risk severity that correlates with healthcare needs and care acuity. This allows providers to prioritize interventions, allocate resources appropriately, and ensure individuals receive the level of care their condition requires.
By systematically evaluating risk factors across body systems and functional domains, the HRST provides a reliable, defensible framework for identifying people at highest risk and informing care decisions. Originally developed and validated for IDD populations, the HRST’s clinical methodology is applicable across other high-risk populations, including people with traumatic brain injury (TBI), physical disabilities, and aging populations receiving long-term services and supports (LTSS).
The result is improved consistency in care delivery, enhanced clinical oversight, and reduced exposure to preventable health complications and outcomes.
The HRST is not an electronic health record (EHR). While EHR systems document health information and services, the HRST provides a validated methodology for identifying and stratifying health risk—delivering clinical insight that complements and enhances the use of EHR data.

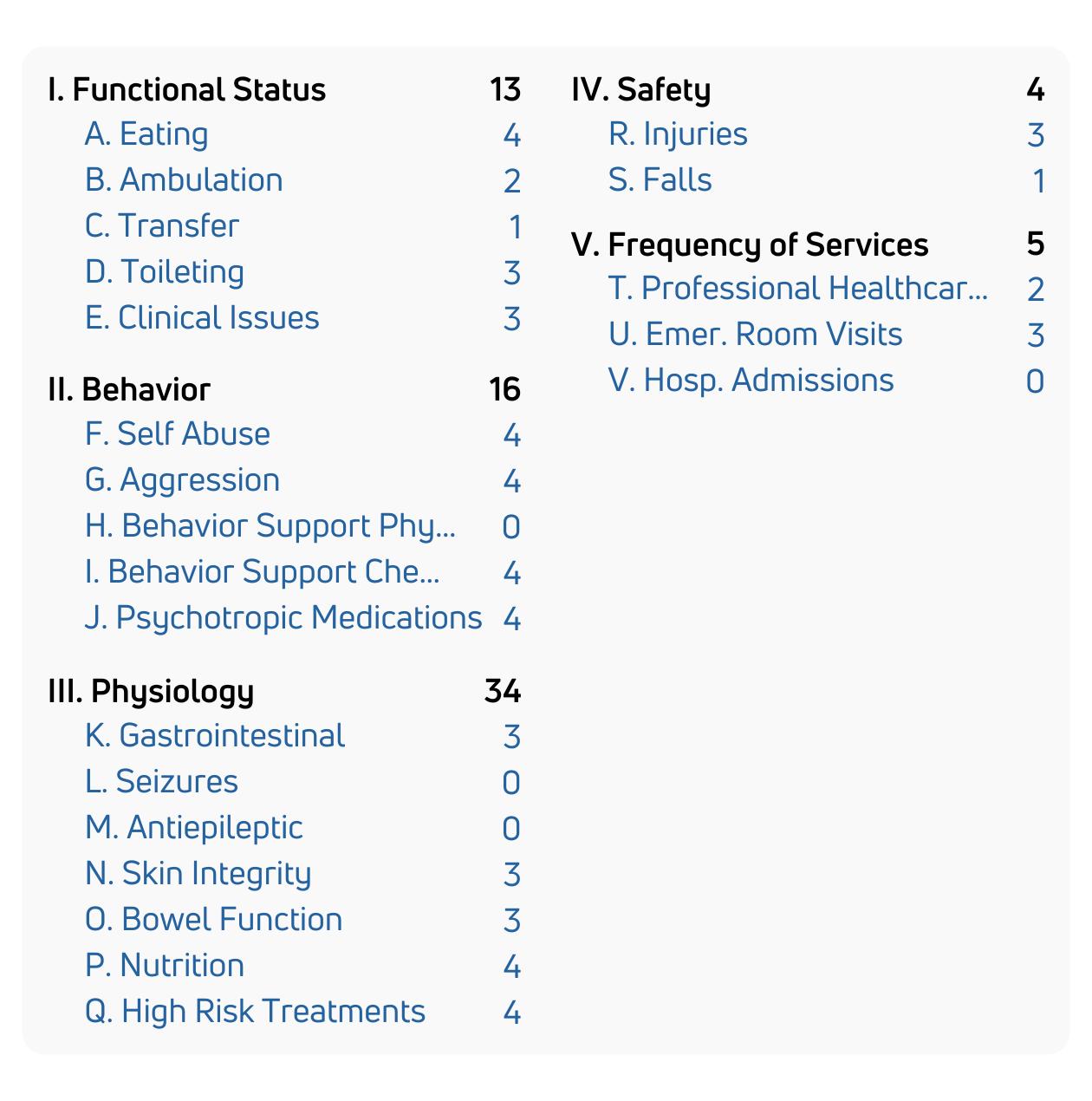
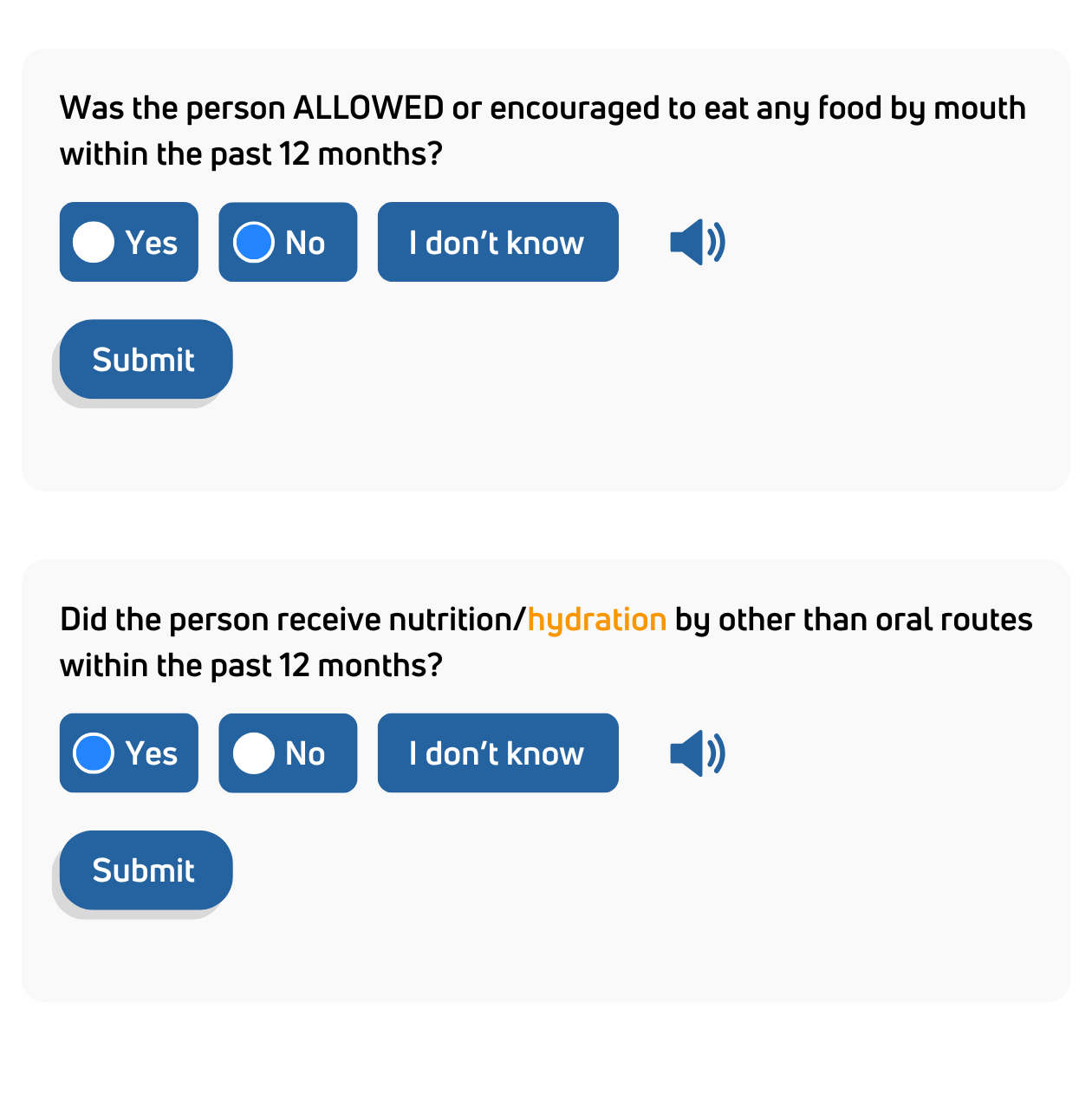
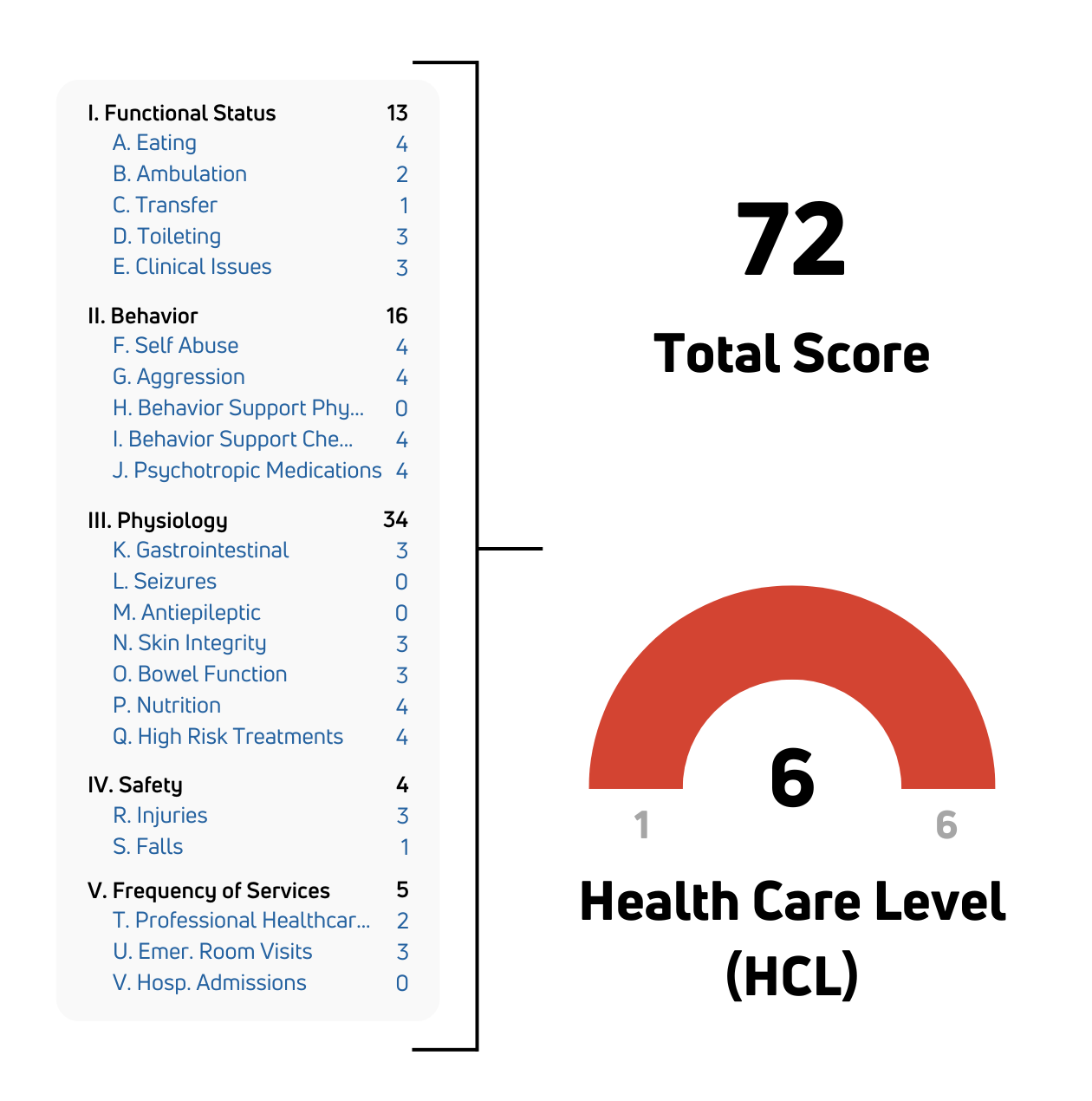
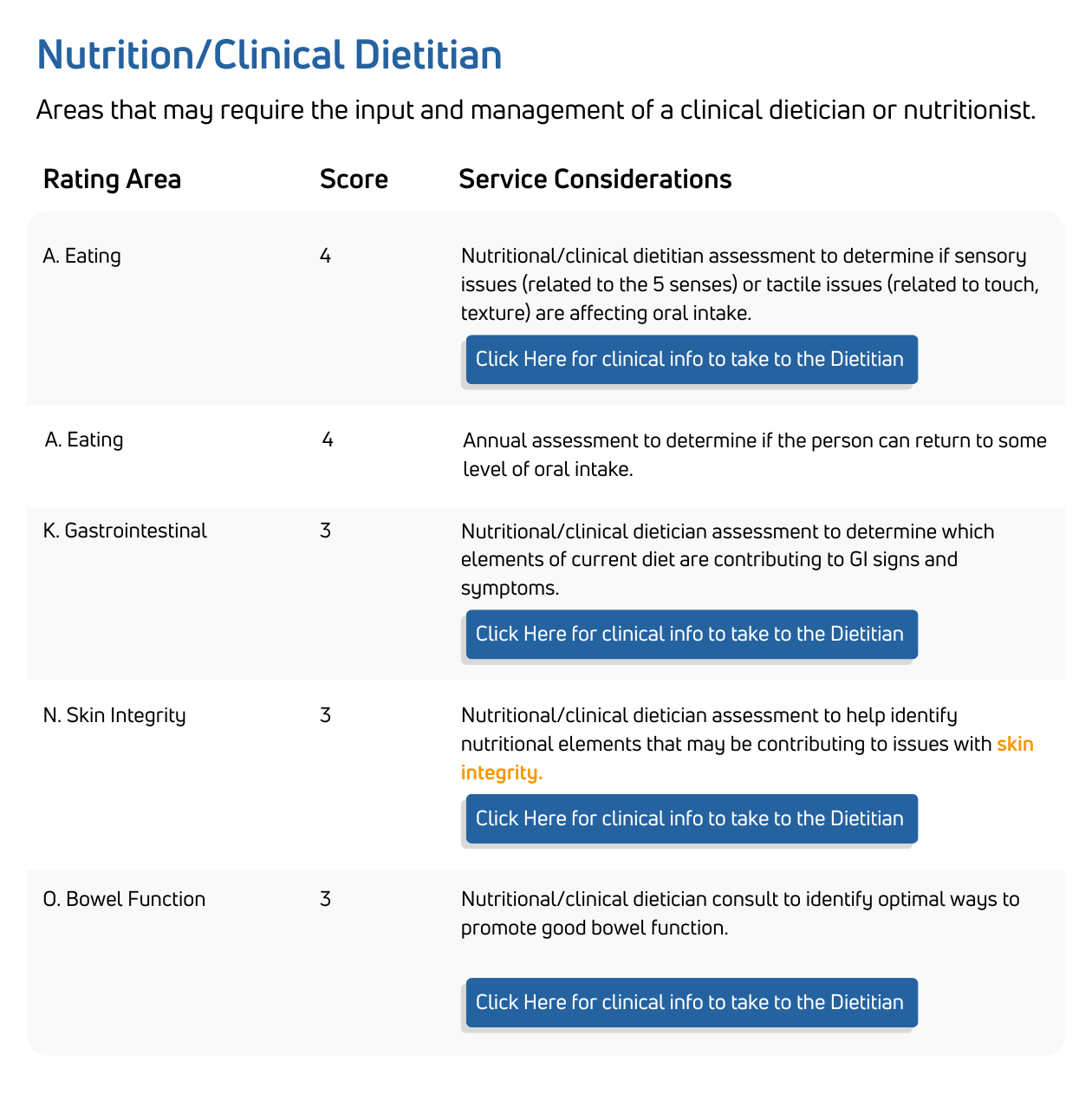



State developmental disabilities agencies use the HRST to ensure people with IDD receive supports and services matched to their actual risk level and clinical acuity, not historical assumptions or administrative categories. The HRST satisfies DOJ settlement agreement requirements, supports waiver-level-of-care determinations, and provides the documented clinical rationale regulators and auditors require. It is also used to inform equitable resource allocation and support rate-setting methodologies aligned to clinical need.
The HRST gives state Medicaid programs a validated, defensible framework to stratify IDD and LTSS populations by clinical acuity and expected utilization, enabling more accurate capitation rate development, actuarial justification, value-based payment structuring, performance-based contracting, and managed care oversight. It provides the clinical intelligence infrastructure that MCO contract accountability requires.
For health plans managing IDD and complex LTSS populations, the HRST operates as a predictive clinical risk engine – surfacing mortality risk, morbidity risk, clinical instability, and acuity level before costs escalate. Earlier identification enables earlier intervention, reduced avoidable ED utilization, fewer inpatient admissions, and measurable improvement in quality metrics and star ratings.
For direct service provider organizations, the HRST translates complex health risk into actionable acuity levels that drive staffing decisions, care planning, and clinical oversight. It identifies developing patterns of risk before they become crises, reducing unnecessary hospitalizations, protecting the people supported from preventable harm, and equipping teams with the clinical confidence to advocate for the resources each person truly needs.