Originally published December 2016. Updated December 2022.
Aspiration occurs when foreign material is inhaled into the airway. Causes of death include asphyxiation due to a blocked airway and irritation or infection of the respiratory tract due to inhaled material, or aspiration pneumonia, which will be the primary focus of this article.
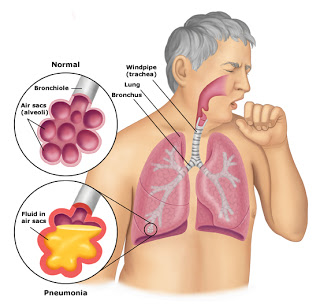
Sources of aspirated material include:
- food or drink
- saliva or nasal secretions
- teeth and dental prosthetics
- objects placed in the mouth, such as gum, toys, coins, or other small foreign objects.
These objects are often contaminated, not only with bacteria from the oral cavity but also with whatever outside organisms they encountered before being placed in the mouth.
Aspirated material can also come from the stomach, either due to vomiting or gastroesophageal reflux (GERD). This material is particularly dangerous because of its elevated acidity.
Factors that enhance the risk of aspiration from either source include:
- altered level of awareness
- poor trunk control
- physical deformity
- medications that are sedating or otherwise impact swallowing
- alcohol consumption
- problems with swallowing, including those associated with the aging process
- behavioral disorders, which involve food seeking/stuffing or consumption of non-food items (PICA)
Recent antibiotic use or hospitalization, place of residence (such as a rehabilitation facility or a nursing home), and overall level of health can also increase the risk for bacterial infection with aspiration pneumonia. Individuals receiving enteral nutrition (tube feeding) have been determined to have a higher level of risk compared with those who eat by mouth.
Statistics are not readily available, but experienced field clinicians say that roughly 25% of the time, the source of aspirated material comes from above, and 75% of the time, it comes from the GI tract.
Symptoms of aspiration include:
- bluish discoloration of the lips or
- coughing or gagging
- discolored, foul-smelling sputum that may contain blood or pus
- chest pain
- shortness of breath
- fatigue
- fever
- wheezing
- sweating without exertion
- breath odor and difficulties with swallowing
Examination findings may reveal fever, elevated respiratory rate, altered respiratory sounds, decreased oxygen saturation, elevated pulse, and decreased mental awareness.
Outcomes with aspiration pneumonia can vary greatly depending on many factors, including the severity and extent of the pneumonia, the type of bacteria involved, and the timeliness of treatment. Individuals who are in poor physical condition at the onset of symptoms will obviously not fare as well as those who are healthier.
Aspiration pneumonia is one of the top causes of death in people with IDD, and it can often be prevented. Decreasing the risk of aspiration pneumonia is a task that must be relentlessly pursued from several angles.
- Simply helping individuals attain optimal body positions during and after eating is a vital first step in the process.
- Specialized support and positioning both during and after a meal may be required for those who have no or poor trunk control or who have other significant bodily deformities such as severe scoliosis.
- The person’s typical response to eating should be known and observed, particularly if they receive enteral nutrition via gastrostomy, jejunostomy, or nasogastric tubes.
- Monitoring for decreased oxygen saturation during and immediately after eating can be a good way to detect silent aspiration.
- People who have known or suspected swallowing disorders, food-related behavioral disorders, and those whose level of awareness may be impacted by medications or other factors should be given particularly close observation and any necessary mealtime support.
- People whose health and nutritional status are compromised should also receive specialized attention and support to decrease their vulnerability.
- Health and safety training for you and direct support staff is important. Ensure consistent and comprehensive knowledge of the warning signs of aspiration pneumonia and the remainder of The Fatal Five.
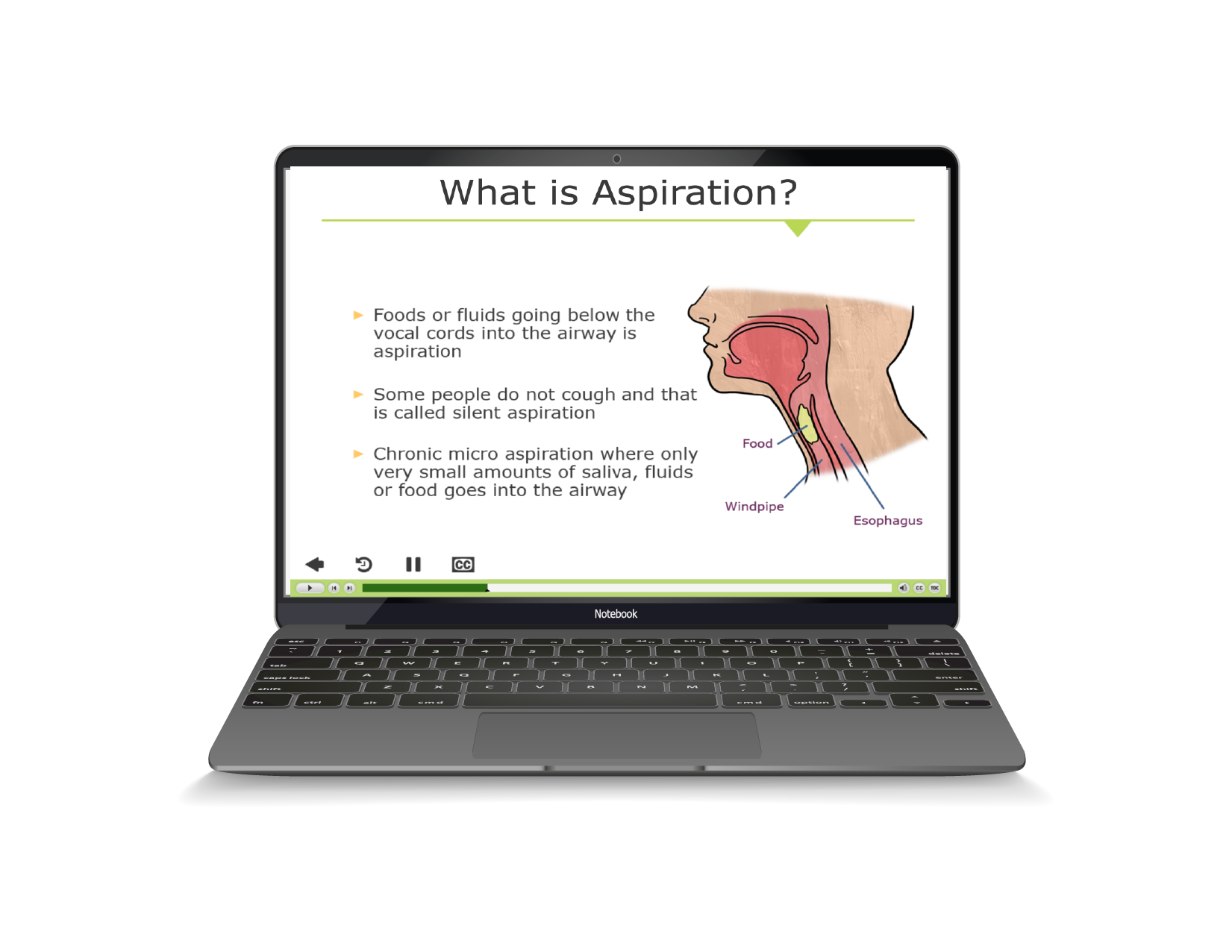
Take the Fatal out of the Fatal Five
License health and safety training eLearns for your entire organization.
Contact us today to receive
a free preview and custom price quote.
