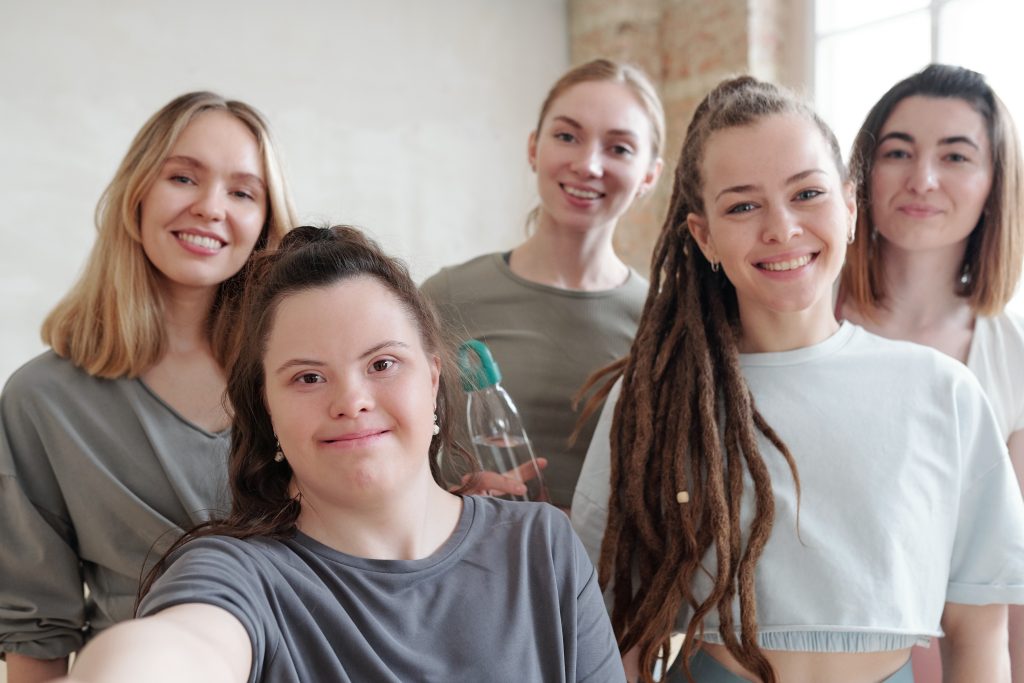Please, May I Have More Data?
By Lorene Reagan
Director of Public Relations, IntellectAbility
Rate-setting considerations for long-term services and supports for people with intellectual and developmental disabilities.
Most actuaries working in the Medicaid space are well acquainted with the acute care rate-setting process. But many may not be familiar with rate setting for Medicaid long-term support and services (LTSS), Home and community-based services (HCBS) for people with intellectual and developmental disabilities (IDD), or the data sources available to inform the rate-setting process. This article introduces the IDD population, their support needs, the most used HCBS services, and the tools that can be used to inform support needs and the IDD-HCBS rate setting process.
Medicaid is the largest funder of LTSS in the U.S. All 50 states and the District of Columbia provide services funded by one or more Medicaid HCBS Waivers, specifically designed to “waive” the provisions within federal Medicaid regulations that historically only paid for services provided in facilities and institutions. Medicaid LTSS waivers allow people with IDD to live in community settings rather than in institutions, facilitating opportunities for community integration and improved quality of life.
According to data published in 2021 by the Institute on Community Integration, an estimated 7.43 million people with IDD live in the United States, and approximately 17% receive services through state IDD agencies. This group’s estimated Medicaid HCBS waiver expenditures were $42.29 billion in 2018.

Some people with IDD live independently in the community and don’t require formal services or support.
Others need support for daily activities such as dressing, bathing, and eating, and for incidental activities such as shopping, cooking, cleaning, and money management. Supports may also be provided to help a person secure and maintain employment, develop relationships, and participate in hobbies, sports, clubs, or worship. There may also be a need for health-related assistance with medications, ambulation, feeding, and other activities to maintain optimal health and manage health risks unique to people with IDD.
Unlike in the past, people with IDD live primarily in community-based settings, not in institutions or nursing homes. Most share a residence with a related family member; some live in group homes, host homes, or adult foster care settings, while others lease or own their own homes.
Services commonly provided under state Medicaid HCBS waiver programs for people with IDD include case management, residential habilitation, community support, personal care, day habilitation, financial management, job coaching, home and vehicle modifications, and assistive technology. Many waivers include self-direct services through which the person selects, hires, and manages their staff and service budget.
Most state Medicaid programs operate their HCBS program for people with IDD using a traditional state-administered Fee-for-Service payment approach, but this is changing with the advent of managed long-term services and supports (MLTSS) programs which employ capitated rates. Unfortunately, there isn’t much experience in this area; while 22 states operated MLTSS programs in 2019, only 10 included the IDD population.
The rate-setting process for HCBS LTSS services is unique and, unlike the approach used in acute care rate setting, focuses mainly on the amount, level, and type of functional, health-related, social, behavioral health, and personal care supports needed for the person with IDD to live successfully in the community.
Each state Medicaid program utilizes the results of various functional screening and assessment tools and other instruments for non-rate setting activities to determine LTSS service eligibility, evaluate level of care, manage health risk, measure acuity, inform resource allocation, and develop service plans. Some are nationally recognized, valid, and reliable instruments and some are “homegrown” tools, having been developed internally. Others are “hybrid” tools based on standardized instruments which the state has customized to meet its unique needs.
In Fee-for-Service programs, states often “tier” LTSS HCBS services. For example, states may have two levels of case management within their Medicaid waiver. A “basic” level and rate are used for people whose needs are more routine, and an “enhanced” level and rate is allowed for those with complex needs, based on assessment findings. In MLTSS, the results of functional assessments and other related data could inform the risk adjustment component of the capitation payment.
As a non-actuary providing subject matter expertise for Medicaid LTSS HCBS rate-setting activities, I learned from my actuary colleagues the value of identifying multiple relevant, valid, and reliable data sources to inform the rate-setting process.
The following are examples of some of the validated tools currently in use that rate-setting teams should consider informing IDD-specific rate setting activities:
- HRST—Health Risk Screening Tool: web-based health risk instrument that identifies health risks, that, if not addressed, are associated with preventable morbidity and mortality in people with IDD. Six levels of risk are assigned.
- SIS-A®—Supports Intensity Scale: Adult Version®: standardized assessment tool designed to measure the pattern and intensity of supports that a person age 16 years and older with IDD requires to be successful in community settings. A numerical Support Needs Index is assigned.
- ICAP—Inventory for Client and Agency Planning: measures adaptive and maladaptive behaviors and is designed for use from infancy to adulthood. Scores that can determine the level of supervision a person needs are generated.
Rate setting for IDD-HCBS is complex and requires multiple inputs and a rate setting team that understands the needs and priorities of people with IDD. Knowing how to select resources that accurately identify support needs, including those required to promote community inclusion and manage maladaptive behaviors, is vital. In addition, because people with IDD have higher incidences of chronic health conditions, lower life expectancies, and difficulty routinely accessing clinically competent healthcare, health risk-related data plays an important role in determining rates. Before selecting the tools to be used in the rate-setting process, the team should evaluate the validity and reliability of each tool and its fitness for use in the rate-setting process.
Published by American Academy of Actuaries – Contingencies. Click here to view the article.